ינהאַלט
דייטינג אַלטראַסאַונד: די 1 אַלטראַסאַונד
The first “meeting” with the baby, the first trimester ultrasound is eagerly awaited by future parents. Also called dating ultrasound, it is also important obstetrically.
The first ultrasound: when does it take place?
The first pregnancy ultrasound takes place between 11 WA and 13 WA + 6 days. It is not compulsory but is one of the 3 ultrasounds systematically offered to expectant mothers and highly recommended (HAS recommendations) (1).
דער קורס פון אַלטראַסאַונד
The first trimester ultrasound is usually done through the abdominal route. The practitioner coats the belly of the mother-to-be with gelled water in order to improve the quality of the image, then moves the probe on the belly. More rarely and if necessary in order to obtain a quality exploration, the vaginal route can be used.
Ultrasound does not require you to have a full bladder. The examination is painless and the use of ultrasound is safe for the fetus. It is advisable not to put cream on the stomach on the day of the ultrasound as this can interfere with the transmission of the ultrasound.
Why is it called a dating ultrasound?
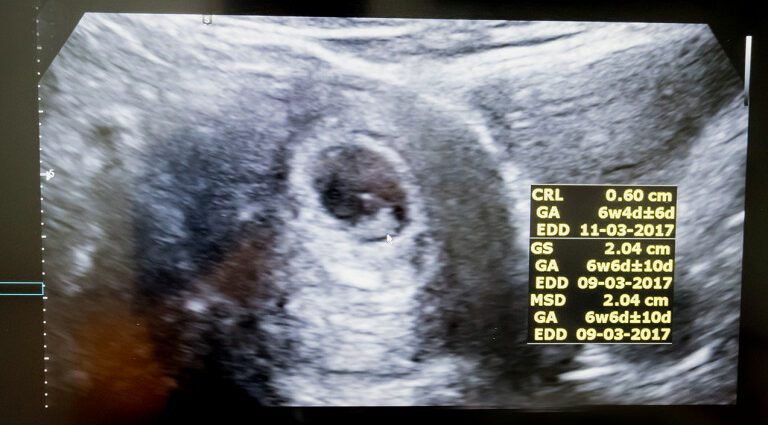
One of the objectives of this first ultrasound is to assess the gestational age and thus date the pregnancy more precisely than the calculation based on the date of the start of the last period. For this, the practitioner performs a biometry. It measures the cranio-caudial length (CRL), that is to say the length between the head and the buttocks of the embryo, then compares the result with a reference curve established according to the Robinson formula (gestational age = 8,052 √ × (LCC) +23,קסנומקס).
This measurement makes it possible to estimate the date of onset of pregnancy (DDG) with an accuracy of plus or minus five days in 95% of cases (2). This DDG will in turn help to confirm or correct the due date (APD).
The fetus at the time of the 1st ultrasound
At this stage of pregnancy, the uterus is still not very large, but inside, the embryo is already well developed. It measures between 5 and 6 cm from head to buttocks, or about 12 cm standing, and its head is about 2 cm in diameter (3).
This first ultrasound aims to check several other parameters:
- the number of fetuses. If it is a twin pregnancy, the practitioner will determine whether it is a monochorial twin pregnancy (a single placenta for both fetuses) or a bichorial (one placenta for each fetus). This diagnosis of chorionicity is very important because it leads to notable differences in terms of complications and therefore of the methods of pregnancy follow-up;
- the vitality of the fetus: at this stage of pregnancy, the baby is moving but the mother-to-be does not yet feel it. He waves, involuntarily, arm and leg, stretches, curls into a ball, suddenly relaxes, jumps. His heartbeat, very fast (160 to 170 beats / minute), can be heard on a doppler ultrasound.
- morphology: the practitioner will ensure the presence of all four limbs, the stomach, the bladder, and will check the cephalic contours and those of the abdominal wall. On the other hand, it is still too much to detect a possible morphological malformation. It will be the second ultrasound, called morphological, to do it;
- the amount of amniotic fluid and the presence of the trophoblast;
- nuchal translucency (CN) measurement: as part of the combined screening for Down’s syndrome (not compulsory but systematically offered), the practitioner measures the nuchal translucency, a fine snore filled with fluid behind the neck of the fetus. Combined with the results of the serum marker assay (PAPP-A and free beta-hCG) and maternal age, this measurement makes it possible to calculate a “combined risk” (and not to make a diagnosis) of chromosomal abnormalities.
Regarding the sex of the baby, at this stage the genital tubercle, that is to say the structure that will become the future penis or the future clitoris, is still undifferentiated and only measures 1 to 2 mm. It is however possible, if the baby is well positioned, if the ultrasound takes place after 12 weeks and if the practitioner has experience, to determine the sex of the baby according to the orientation of the genital tubercle. If it is perpendicular to the axis of the body, it is a boy; if it is parallel, a girl. But beware: this prediction has a margin of error. Under the best conditions, it is only 80% reliable (4). Doctors therefore generally prefer to wait for the second ultrasound in order to announce the sex of the baby to the future parents, if they wish to know it.
The problems that the 1st ultrasound can reveal
- אַ מיסקעראַדזש : the embryo sac is there but there is no cardiac activity and the measurements of the embryo are lower than normal. Sometimes it is a “clear egg”: the gestational sac contains the membranes and the future placenta, but no embryo. The pregnancy ended and the embryo did not develop. In the event of miscarriage, the gestational sac may evacuate spontaneously, but sometimes it is not or incompletely. Medicines are then prescribed to induce contractions and promote the complete detachment of the embryo. In case of failure, surgical treatment by aspiration (curettage) will be carried out. In all cases, close monitoring is necessary to ensure the complete evacuation of the product of pregnancy;
- אַן עקטאָפּיק שוואַנגערשאַפט (GEU) or ectopic: the egg did not implant in the uterus but in the proboscis due to a migration or implantation disorder. GEU usually manifests early in progression with lateral lower abdominal pain and bleeding, but sometimes it is discovered incidentally during the first ultrasound. GEU can progress to spontaneous expulsion, stagnation or growth, with a risk of rupture of the gestational sac which can damage the tube. Monitoring with blood tests to assay the beta-hcg hormone, clinical examinations and ultrasounds makes it possible to monitor the evolution of GEU. If it is not at an advanced stage, treatment with methotrexate is usually sufficient to cause expulsion of the gestational sac. If it is advanced, a surgical treatment by laparoscopy is performed to remove the gestational sac, and sometimes the tube if it has been damaged;
- better than normal nuchal translucency is often seen in babies with trisomy 21, but this measure should be included in the combined screening for trisomy 21 taking into account maternal age and serum markers. In the event of a combined final result greater than 1/250, it will be suggested to establish a karyotype, by trophoblast biopsy or amniocentesis.